All oral health articles
342 results

Fluoride
Who Should Use a Fluoride Mouth Rinse and Why?
We often think of mouthwash or mouth rinse as our go-to for a minty fresh kiss or whiter smile.
Read More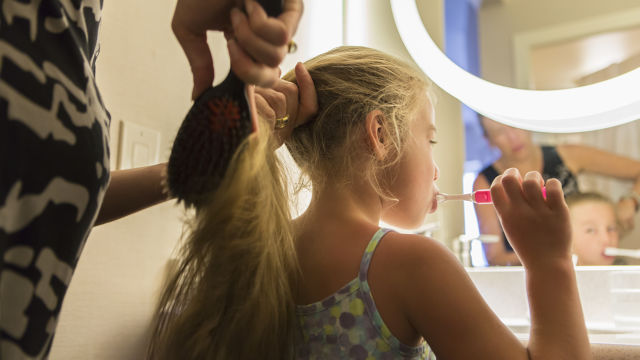
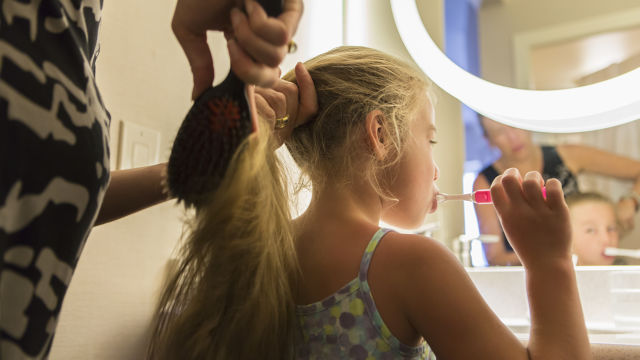




Fluoride
What Is Stannous Fluoride Toothpaste?
Fluoride is a cornerstone of dental health, commonly found in oral care products we use at home. While you may be familiar with types like sodium fluoride, this article dives into stannous fluoride, also known as tin (II) fluoride.
Read More
Bad Breath (Halitosis)
How To Tell If You Have Bad Breath
Learn how to identify if you have bad breath and discover practical tips on how to stop smelly breath for a fresher, more confident feeling. Learn more now."
Read More


Bad Breath (Halitosis)
How To Manage Alcohol Breath
Drinking too much alcohol is bad news for your body and also for your breath. Find out how you can manage and get rid of alcohol breath here.
Read More
Bad Breath (Halitosis)
What Causes Morning Breath and How to Prevent It
Learn how to prevent morning breath with our effective tips. Discover the underlying causes and find effective strategies to wake up feeling fresh and confident.
Read More
Bad Breath (Halitosis)
What To Do About Chronic Bad Breath
If you have chronic bad breath (halitosis), you know how embarrassing this problem can be. Instead of using breath mints & gum, get to the root of the issue.
Read More
Bad Breath (Halitosis)
Can A Sinus Infection Cause Bad Breath?
When it comes to a sinus infection, bad breath is often a side effect, as the sinuses drain into the back of your throat. Luckily, this condition is treatable.
Read More


Bad Breath (Halitosis)
How to Control Bad Breath: A Comprehensive Guide
Learn about essential oral hygiene tips, including proper dental flossing, as part of your effective bad breath treatment plan. Read more at Colgate AU now.
Read More



Bad Breath (Halitosis)
How to Get Rid of Bad Breath
Learn how to get rid of bad breath and discover effective strategies, from advanced oral hygiene to professional treatments, for a lasting cure and confident smile.
Read More
Bad Breath (Halitosis)
Halitosis: Causes of Bad Breath
Explore the common bad breath causes, from diet to underlying health issues. Learn what leads to chronic bad breath & how to identify it for effective treatment.
Read More
Bad Breath (Halitosis)
Effective Home Remedies for Bad Breath
Explore home remedies for bad breath. Learn natural ways to freshen your breath with simple tips like salt water rinses & tongue scraping for lasting freshness.
Read More

Bad Breath (Halitosis)
Trouble with Tonsil Stones and Bad Breath
What's the deal with tonsil stones? Bad breath, irritation and a whitish spot at the back of your throat are a few signs that you have a tonsil stone.
Read More


Cavities
4 Home Toothache Remedies
Looking for toothache relief? Explore 4 effective homemade remedies to reduce toothache pain and find comfort. Simple solutions for sensitive teeth and general aches.
Read More




Cavities
Reverse & Prevent Tooth Decay: Your 5-Step Guide
Discover effective ways to reverse early tooth decay and prevent cavities. Learn actionable tooth decay treatment tips for a healthier, stronger smile.
Read More

Cavities
Protecting Your Enamel & Preventing Tooth Decay
Understand how bacterial acid leads to enamel loss and tooth decay. Discover proven methods to prevent cavities and keep your tooth enamel strong and resilient
Read More
Cavities
What Are Incipient Caries?
Incipient caries is the beginning stage of tooth decay. Find out more about incipient caries and learn how you can stop decay in its tracks and avoid the drill.
Read More
Cavities
Tooth Decay Stages: From Enamel Damage to Cavities
Learn the stages of tooth decay, from initial enamel damage & tooth enamel erosion to advanced cavities. Learn what happens at each phase for better oral health.
Read More
Cavities
Cavity Symptoms: How to Detect Cavity & Tooth Decay
earn to spot the early signs of a cavity and tooth decay. Recognizing these symptoms quickly can help prevent further damage and ensure timely treatment.
Read More
Cavities
What Is a Root Cavity and How Can You Prevent It?
A root cavity occurs on the root of your tooth rather than the enamel. Learn more about how to prevent and treat this type of cavity.
Read More




.jpeg)
Dry Mouth
What is Dental Cottonmouth?
What is cottonmouth? This condition occurs when your salivary glands don't make enough saliva to keep your mouth wet. Find out more about cottonmouth here.
Read More.jpeg)
Dry Mouth
How to Manage Dry Mouth at Night for Better Sleep
Struggling with dry mouth at night? Discover common causes and effective management tips to find relief and improve your sleep and oral health.
Read More
Dry Mouth
How Do Dry Mouth Lozenges Work?
Saliva plays an important role in keeping your mouth healthy. If you have a dry mouth, dry mouth lozenges may help stimulate your saliva production.
Read More


Dry Mouth
Dry Mouth Toothpaste 101: What Is It & How Does It Work?
Dry mouth toothpastes can stave off discomfort and potential health issues. Find out if dry mouth toothpastes can relieve your dry mouth (xerostomia)
Read More








Mouth & Teeth Anatomy
The Oral Cavity: Parts, Functions & Importance for Health
Explore the oral cavity anatomy: learn about the different parts of your mouth and their vital functions in speaking, eating, and maintaining oral health.
Read More
Mouth & Teeth Anatomy
How to Get Rid of a Dry Throat | Colgate®
Wondering how to get rid of a dry throat? Learn about some of the common causes, including allergies, dehydration, the common cold and more.
Read More

Mouth & Teeth Anatomy
Do You Know All The Human Teeth Names?
Get a better understanding of the human teeth names, each tooth's location in the mouth and how you use them in daily functions.
Read More











Teeth Whitening
Understanding Teeth Stains: Causes & Removal Methods
Concerned about teeth discoloration or brown stains on teeth? Learn different types of teeth stains & their effective removal methods for a brighter smile.
Read More
Teeth Whitening
Build Your Best At-Home Tooth Whitening Kits
When you're on holiday, you don't want to slack off on your tooth-whitening or oral healthcare regime.
Read More
Teeth Whitening
Top Tips to Whiten Yellow Teeth Naturally
Discover top tips on how to whiten yellow teeth naturally and effectively. Learn simple methods to brighten your smile from the comfort of your home.
Read More


Teeth Whitening
Banana Peel Teeth Whitening: Will It Give You A Brighter Smile?
Some claim that banana peel teeth whitening works, but does the science support it? Learn more about bananas and what you can do for a whiter smile, here.
Read More
Teeth Whitening
What are teeth whitening options if you have a crown?
Can you whiten a crown when you've had dental work and want to brighten your smile? Before you proceed, it's best to speak with your dentist about your options.
Read More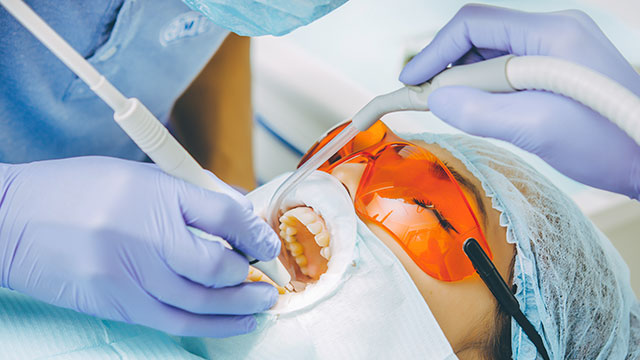
Teeth Whitening
What are the best Instant Teeth Whitening Options?
Here are your options, including the fastest teeth whitening treatments, and the ones that take some time.
Read More
Teeth Whitening
4 Types Of Teeth Whitening Products
The primary factors that dictate what patients want in teeth whitening are ease of application, effectiveness and affordability.
Read More

Teeth Whitening
What Works Best To Remove Coffee Stains From Your Teeth?
Most of us can't live without a daily dose of coffee to jump start the day, but could the beverage that puts morning smiles on… Read more at Colgate.com
Read More
Teeth Whitening
Burned Gums from Teeth Whitening: What You Need to Know
If you’ve ever burned the inside of your mouth on a hot pizza slice, you know that irritating your oral cavity’s soft tissue is no laughing matter.
Read More
Teeth Whitening
What Are the Different Types of Teeth Whitening Products?
Are you considering teeth whitening? A bright, white smile is an essential goal for many and is often considered the focus of their oral care routine.
Read More
Teeth Whitening
How Does a Teeth Whitening Pen Work?
Teeth whitening pens are the perfect solution for anyone looking to get whiter teeth. Learn about how they work, the benefits of using them, and how to use them
Read More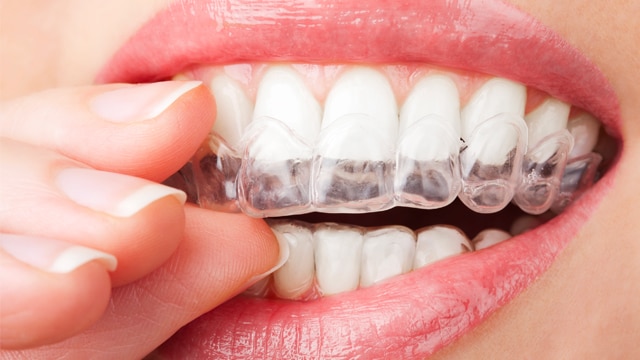
Teeth Whitening
How Custom Whitening Trays Brighten Your Smile
If your teeth aren't as white as you'd like, there are safe and simple ways to improve them. One is the use of custom whitening trays.
Read More
Teeth Whitening
3 Tips For Preventing Teeth Stains From Braces
Learn about our top 3 tips for preventing stained teeth from braces and whitening your teeth evenly when your braces come off.
Read More
Teeth Whitening
Is LED Teeth Whitening Right For You?
LED teeth whitening is a popular option for achieving a brighter smile. The process is relatively comfortable and convenient, and can offer great results. But is it the best at-home treatment for you?
Read More
Teeth Whitening
Is The Cost Of Professional Teeth Whitening Worth It?
If you've considered whitening your teeth, you may already know the professional teeth whitening cost can be higher than at-home alternatives. Learn more here.
Read More
Teeth Whitening
Hydrogen Peroxide for Teeth Whitening: Does it Work and is it Safe?
Find out the truth about hydrogen peroxide teeth whitening, whether it can really work, if it is safe to use on your teeth, and how to use it correctly!
Read More
Teeth Whitening
Best Methods for Keeping Teeth White With Braces: Get Glowing Results
Just because you have braces doesn't mean that you can't improve the quality of your smile.
Read More
Teeth Whitening
How Does LED Teeth Whitening Work?
LED teeth whitening is a new and impressive way to achieve brighter teeth. It uses LED lights to activate the whitening solution, resulting in whiter teeth in a shorter amount of time.
Read More
Teeth Whitening
How Hydrogen Peroxide Effectively Whitens Teeth
Having a bright and radiant smile is a desire for many individuals. People often turn to whitening products to whiten their teeth.
Read More
Teeth Whitening
Is Hydrogen Peroxide safe for teeth?
When it comes to achieving a bright and dazzling smile, many individuals turn to teeth whitening methods to enhance their pearly whites.
Read More
Teeth Whitening
What Causes Green Tooth And Other Tooth Discolouration?
Tooth discolouration like a green tooth can occur for a number of reasons and can really impact your confidence. Here's why it happens and what to do.
Read More
Teeth Grinding (Bruxism)
Bruxism: Signs and Symptoms
Bruxism, Bruxism Symptoms & Sleep Bruxism | Colgate AU
Read More
Teeth Grinding (Bruxism)
Night Guard For Teeth Grinding: A Simple Treatment Method
How To Wear A Night Guard For Teeth Grinding | Colgate AU
Read More

Teeth Grinding (Bruxism)
Teeth Grinding: How to Stop Grinding Your Teeth at Night!
How to Stop Teeth Grinding at Night: Symptoms and Treatments
Read More
Oral Care: Kids (5-12)
Early Childhood Cavities: What Parents Need to Know
Understand early childhood cavities: their causes, how to prevent them, and essential care tips. Protect your child's developing smile from decay.
Read More



Oral Care: Kids (5-12)
Can Kids Use Mouthwash? Safety & Benefits for Young Smiles
Guide to kids mouthwash and safety. Find out what age can kids use mouthwash, the benefits of fluoride mouthwash & expert tips for protecting your child's smile.
Read More
Oral Care: Kids (5-12)
Healthy Kids’ Teeth: Laying The Foundation For Lifelong Oral Health
Read More

Oral Care: Kids (5-12)
4 Healthy Habits for Your Kids' Oral Care
Children learn by example and setting up great oral hygiene habits is one of the best things that you can do for your child’s oral health.
Read More


Oral Care: Kids (5-12)
9 Causes of Bad Breath in Babies & Toddlers
Even healthy children can sometimes experience bad breath (halitosis). If you've noticed that your little one's breath is not so pleasant, there is hope.
Read More
Oral Care: Kids (5-12)
What to Do for a Child With a Toothache? | Colgate®
Most of the time, a toothache is caused by injury to the tooth or a cavity. Here are some things that you can do to help your child if they have a toothache.
Read More
Oral Care: Kids (5-12)
Space Maintainers Help With a Perfect Smile
Space maintainers are a dental device used for children as they lose teeth and wait for adult teeth to grow in.
Read More
Oral Care: Kids (5-12)
Top Teething Remedies For Babies: Helping Your Little One Overcome The Pain
When your baby's first tooth breaks through the gums, you have both reached an exciting milestone. But it could be a painful one. These remedies can help.
Read More

Oral Care: Kids (5-12)
How to Care for Your Toddler's Teeth: Brushing & Beyond
Learn how to care for your toddler's teeth effectively. Our guide covers how to brush baby teeth and essential routines for a healthy, developing smile
Read More


Oral Care: Kids (5-12)
Australian Kids Talk Teeth
Ever wondered what Australian kids think of the tooth fairy, or where their teeth come from? Watch this video for a fun discovery of the world of teeth from a whole new perspective.
Read More
Oral Care: Kids (5-12)
How Do I Know If My Baby Is Teething? Signs, Remedies & Tips
Learn what age do babies start teething, the first signs and effective teething tips to comfort your baby. Find advice on how to help with teething and remedies.
Read More
Oral Care: Kids (5-12)
What Causes White Spots on Baby Teeth?
Worried about white spots on baby teeth? Learn common causes of white spots like fluorosis, tooth decay, and what they mean for your child's dental health.
Read More
Oral Care: Kids (5-12)
When To Take Your Child To The Dentist For The First Time
When should your child’s first dental visit be? The Australian Dental Association says when the first tooth erupts in the mouth.
Read More
Tooth Extraction
Tooth Removal / Tooth Extractions
Many dentists recommend extracting impacted teeth that are only partially erupted.
Read More
Tooth Extraction
Dry Socket After Tooth Extraction: Understanding And Prevention
Dry Socket After Tooth Extraction: Understanding And Prevention
Read More
Tooth Extraction
Tooth Extraction And Dry Sockets
Wisdom teeth, or third molars, are often extracted. Some people naturally have enough room in their mouths to accommodate the eruption of wisdom teeth.
Read More
Tooth Extraction
Serious Tooth Infections
The pain from a toothache can be debilitating, and it's usually an indication of a deeper issue such as tooth infection.
Read More
Dental Product Guidance
How do Colgate Mouthwashes Work?
Colgate® mouthwashes are uniquely designed to amplify the benefits of brushing. When used together, a toothbrushing and mouthwash system expands the potential for oral care.
Read More
Dental Product Guidance
Benefits and Features of an Electric Toothbrush
Tooth brushing needs our full attention! However, if interest or ability is lacking, an electric toothbrush is a great alternative to a traditional toothbrush.
Read More







Dental Product Guidance
Is Flossing Hard? Interdental Brushes May Be The Answer
According to Better Health, cleaning in between the teeth and around the gumline is essential for maintaining good oral health and preventing gum disease.
Read More



Dental Product Guidance
Should You Consider a Water Flosser?
Flossing is important for good oral health. If you have difficulty using string floss, talk to your dentist about alternatives, like a water flosser.
Read More


Dental Product Guidance
Basics Of Brushing For Kids: What Toothpaste Is Right For Your Toddler?
Read More
Dental Product Guidance
Are Electric Toothbrushes Better Than Manual Toothbrushes?
Electric or Manual Toothbrushes, which one is better? Learn their differences, considering their effectiveness in dental health and oral hygiene.
Read More
Dental Product Guidance
How Electric Toothbrushes Help With Receding Gums
Know how Electric toothbrushes help prevent receding gums and improve oral health. Learn brushing techniques & tips from Colgate.
Read More
Dental Product Guidance
Your Guide to using Electric Toothbrushes For Braces
Electric toothbrushes are a fantastic investment into your oral health, especially if you wear braces. Learn about electric toothbrushes for braces in this guide.
Read More
Dental Product Guidance
How to Build a Healthy Oral Care Habit with a Timed Electric Toothbrush
Getting the perfect oral care routine can be difficult. Timed electric toothbrushes can help you stay on track. Learn how from Colgate.
Read More
Dental Product Guidance
Do electric toothbrushes whiten teeth better than manual toothbrushes
Wondering if you should switch to an electric toothbrush to help whiten your teeth better than a manual toothbrush? Read to know how well they work!
Read More








Mouth Sores and Infections
What A Gum Boil Could Mean For Your Dental Health | Colgate®
If you notice anything strange in your mouth, like a gum boil or a bump that looks like a pimple, it's a good idea to have it checked out by a dentist.
Read More





Dental Health Threats
How Mouth Spray Helps Dry Mouth
A dry mouth spray may be good option if you need short-term relief of dry mouth. Learn how sprays work and what you can do for longer-term solutions, here.
Read More



Dental Visits
Overcoming Fear and Anxiety at the Dental Clinic
Don't worry! This is common, but we're here to share some tips and advice to help you fight the fear and get back in the chair. Learn more here.
Read More


Veneers
How Porcelain Dental Veneers Can Rebuild Your Smile
People with healthy smiles like to show them off, but for people with chipped, discoloured or crooked teeth, smiling can be a painful experience, emotionally and physically.
Read More
Veneers
Pros and Cons of Dental Veneers
Dental veneers are thin pieces of tooth-coloured porcelain or composite resin material that are bonded to the facial (front) surfaces of your natural teeth.
Read More





Oral Care: Adults (18+)
What is Good Oral Hygiene?
Good oral hygiene results in a mouth that looks and smells healthy.
Read More
Oral Care: Adults (18+)
Ten Causes of Yellow Teeth and How to Avoid Them
Yellow teeth can cost you your confidence and propensity to smile every day. Here are ten common causes of this undesirable tinge and how to avoid it.
Read More
Oral Care: Adults (18+)
What is Referred Tooth Pain and What Causes It?
Not all teeth pain originates in the tooth itself. Discover the concept of referred tooth pain, its sources & why understanding it is crucial for diagnosis.
Read More



Oral Care: Adults (18+)
Choosing The Best Toothbrush For Braces
When you or your child are wearing braces, maintaining good oral health is more important than ever.
Read More











Pregnancy Oral Care
Relief For Dry Mouth During Pregnancy
What can you do about a dry mouth (xerostomia) during pregnancy? It's not as commonly discussed as other symptoms but that dry feeling can accompany nausea...
Read More
Pregnancy Oral Care
Toothache During Pregnancy? Why It Happens & Safe Ways to Find Relief
To avoid a toothache during pregnancy, or any other dental problem when expecting a baby, your best strategy starts with a dental visit.
Read More
Pregnancy Oral Care
Bleeding Gums During Pregnancy: Causes, Symptoms & Safe Treatment
Experiencing sore gum during pregnancy? Learn the causes of bleeding gums, effective pregnancy gingivitis treatment & essential oral care tips for expectant mothers.
Read More
Root Canals
Do I Need A Root Canal Filling?
If you have been experiencing problems with a tooth, you may wonder, "Do I need a root canal filling?" Root canal fillings, also known as endodontic therapy, are performed when the nerve or pulp of the tooth becomes infected
Read More

Root Canals
Myths About Root Canal Treatment
When people are told that they need a root canal therapy, they often worry that it's going to be painful.
Read More
Root Canals
A Step-by-Step Guide To Root Canal Therapy
The goal of the root canal therapy is to save a tooth that is severely infected. As Dental Health Services Victoria puts it, a dentist performs the procedure to replace damaged or infected pulp in the tooth's root canal with a root filling.
Read More

Plaque & Tartar
What is Tartar?
Tartar, sometimes called calculus, is plaque that has hardened on your teeth.
Read More





Digestive (Gastrointestinal) Disorders
Bad Breath From Stomach Problems
Bad breath can come from a number of places, but did you know you can get bad breath from stomach problems?
Read More
Digestive (Gastrointestinal) Disorders
Why Am I Getting Heartburn While Pregnant? Guide to Acid Reflux in Pregnancy
Your guide to acid reflux in pregnancy. Explore causes of acid reflux, effective home remedies and essential oral care strategies to safeguard your smile. Read now.
Read More
Digestive (Gastrointestinal) Disorders
Acid Reflux: A Dental Disaster In The Making
You take your child to their dental appointment, expecting smiles all around and a clean bill of health.
Read More
Bridges & Crowns
What are Dental Crowns and Tooth Bridges?
Both crowns and most bridges are fixed prosthetic devices. Unlike removable devices such as dentures, which you can take out and clean daily, crowns and bridges are cemented onto existing teeth or implants, and can only be removed by a dentist.
Read More








Dentures
How To Clean Dentures To Avoid Bacteria Buildup
Learning how to clean dentures is important for maintaining good daily hygiene, but occasionally you may need to take these extra steps.
Read More





Nutrition & Oral Health
Is Milk Good For Your Teeth? | Colgate®
We know that dairy keeps your bones strong and healthy, but is milk good for your teeth? The answer is a resounding yes, and here's why.
Read More

Brushing & Flossing
How to Floss Correctly
Master dental flossing with our easy guide. Learn how to floss correctly to remove plaque, prevent cavities, and improve gum health for a healthier smile.
Read More





Brushing & Flossing
Can an Electric Flosser Make Flossing Easier?
Flossing is an essential part of an oral hygiene routine, but it can be difficult for some people. An electric flosser might make the task easier.
Read More
Brushing & Flossing
7 Essential Tips to Keep Your Teeth Healthy
Elevate your dental health with seven easy-to-follow practices. Embrace gentle dental care routines for a lifetime of healthy teeth and a confident smile.
Read More
Brushing & Flossing
How Long Should I Brush My Teeth? Answering Your Toothbrushing Questions
The key to preventing and controlling gum disease is brushing at the gum line where bacteria and plaque tend to accumulate. Learn more here.
Read More






Gum Disease (Gingivitis)
Understanding the 5 Common Causes of Bleeding Gums
Explore 5 causes of bleeding gums you should know. Learn why your gums bleed, from gingivitis to brushing habits & what steps to take next for healthier gums.
Read More.png)
Gum Disease (Gingivitis)
Gingivitis Treatment: Steps for Healthier Gums
Learn how to fight gingivitis with three simple steps, integrating home care & professional dental visits. Understand gingivitis causes and when to see a dentist.
Read More
Gum Disease (Gingivitis)
Can Receding Gums Grow Back?
Gum recession happens for a number of reasons, such as brushing your teeth with too much pressure. Learn more about what causes gums to recede and how to manage it here.
Read More

Gum Disease (Gingivitis)
Periodontal Surgery — What Do I Need to Know?
After gum surgery, it is important that the periodontist or dental hygienist inform you how to clean the teeth and gum tissue with a toothbrush and an antimicrobial fluoride toothpaste, floss or interdental device and antibacterial mouth rinse.
Read More



Gum Disease (Gingivitis)
Gum Disease Symptoms And What To Do About Them
By familiarising yourself with gum disease symptoms, you can get proper care immediately if you develop a problem.
Read More
Gum Disease (Gingivitis)
What Is Trench Mouth?
One of the most painful types of gum disease is called trench mouth. The name dates back to World War I. Find out more about trench mouth here.
Read More
Gum Disease (Gingivitis)
Periodontal Charting: What It Is & Why It's Important
Have you ever noticed the dental hygienist or dentist taking measurements of your gums? That's periodontal charting, a part of preventative oral care.
Read More
Gum Disease (Gingivitis)
Bleeding Gums Treatment and Home Remedies
Bleeding gums when you brush or floss are often an early symptom of gum problems, which can lead to more serious issues.
Read More
Gum Disease (Gingivitis)
What is Gingivitis: Signs & Symptoms
understand what gingivitis is, its causes, and how to recognize its symptoms. Spot the warning signs early to protect your gums and maintain optimal oral health.
Read More
Gum Disease (Gingivitis)
Gingivectomy Surgery: What You Need To Know
A gingivectomy may be performed to remove excess gum tissue or to shape the gums for easier cleaning or restoration of the teeth. Learn more here.
Read More
Gum Disease (Gingivitis)
Why Do You Have Itchy Gums?
The most likely reason for your itchy gums is plaque. Check-in with your dentist so they can properly examine your gums and teeth.
Read More
Gum Disease (Gingivitis)
Periodontal Disease & How You Can Prevent It
Have you experienced tender or bleeding gums? Know the causes, treatments and steps to prevent gum disease.
Read More
Gum Disease (Gingivitis)
How Teeth Cleaning Helps Prevent Gum Disease
Gum disease is a very common infection. Getting a teeth deep cleaning can remove the infection, plaque and tartar so that your gums can heal.
Read More
Tooth Sensitivity
How to Reduce Tooth Sensitivity: Treatment Tips
Find out how to reduce tooth sensitivity with various treatment options. From daily care to addressing tooth erosion, discover effective ways to manage discomfort.
Read More



Tooth Sensitivity
What Causes Tooth Sensitivity: The Science Behind the Pain
Learn why you experience tooth sensitivity. Discover how exposed dentin and other factors like gum recession or enamel erosion lead to that sharp, sudden pain.
Read More
Tooth Sensitivity
Sensitive Teeth After Cleaning: What to Expect & How to Cope
find out why teeth are sensitive after cleaning. Get immediate tips on how to stop sensitive teeth pain immediately and manage any post-cleaning gum bleeding.
Read More







Oral Care: Babies (0-4)
Common Teething Symptoms: A Parent's Guide
Learn to identify the most common teething symptoms in babies. Understand what to look for to help soothe your child's discomfort during this developmental stage
Read More

























Adult Orthodontics
Adults and Braces
Explore modern adult braces options, from traditional to discreet clear aligners. Discover how orthodontic treatment can improve your oral health & confidence.
Read More

Adult Orthodontics
Types of Braces: Your Orthodontic Options
Explore different types of dental braces: metal, ceramic, lingual & more. Understand each braces type's pros, cons & suitability for your orthodontic journey.
Read More
Adult Orthodontics
What Are Lingual Braces?
Discover what lingual braces are, how they work, and their unique benefits for discreet teeth straightening. Learn if these hidden braces are right for you.
Read More
Adult Orthodontics
Choosing Ceramic Braces: What You Need to Know
Explore ceramic braces, often called white braces, for a less noticeable orthodontic treatment. Understand their advantages & if they align with your lifestyle.
Read More




















Cancer
Early Signs Of Mouth Cancer
According to the Australian Dental Association, half of those affected by oral cancer in Australia survive after five years.
Read More





Early Orthodontics
Maintaining Your Smile: The Importance of Retainers After Braces
Understand the crucial role of a retainer after braces. Discover various types and how proper maintenance helps preserve your orthodontic results.
Read More










